There is a lot unknown right now about how the COVID-19 pandemic will impact higher education’s future. One thing is known for sure, though: campuses will adapt into new ways of teaching and learning. Here, we’re taking a closer look at how the pandemic will impact health sciences programs. While these factors are already integrated into many programs, they will become even more critical to training our future healthcare workforce.
Adapting Health Sciences Education Post-COVID
by Larry Schnuck, AIA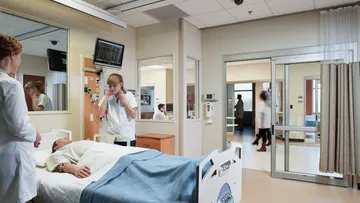

Increased Demand for Health Professionals and Health Sciences Programs
For several years, every state in our country has tracked and felt the effects of the decline in nurses and other health professionals entering the workforce. As colleges and universities recover from months of closed campuses, many campuses are already seeking opportunities to expand their programs to meet the COVID-19 crisis needs. The pandemic has revealed to future students the importance and vital role of healthcare workers. Many will be influenced by stories that come out of this time, and therefore may be inspired to pursue careers in these professions. The World Health Organization’s recent publication State of World’s Nursing 2020: Investing in Education, Jobs and Leadership report recommends “to invest in a massive acceleration of nursing education, create at least 6 million new nursing jobs by 2030 and strengthen nurse leadership.” Additionally, several campuses around the country have already announced either adding new or expanding nursing and health sciences programs in response to increased interest since the pandemic. As colleges and universities seek ways to recover, investments in these programs may help to ensure a viable future for not only higher education but also for the health of our communities.

Interdisciplinary Education is Here to Stay
Around the country, college programs have recognized and embraced the idea that our future healthcare practitioners need to train as integrated care teams in order to best prepare them for the working world. As our country has witnessed firsthand these past months, nurses, doctors, respiratory therapists and an entire multitude of specialties must come together to treat patients. Therefore, as health science programs resume, we encourage them to continue to push boundaries for training these students to work side-by-side. How can you, as a higher education organization, shift your pedagogies to encourage interaction between programs? Once back on campus, how can you share laboratories and resources to maximize exposure of students to different collaborative specialties? For more ideas on how to integrate these types of changes for your facilities, see our American School & University article “Interprofessional Education: Creating Spaces that Foster Collaboration and Understanding”.

Experiential Learning: Simulation Will Help Fill the Gap
It remains unclear when and with what restrictions clinical sites may open for needed student training hours. Already, simulation labs are being heavily relied upon by programs to offer students opportunities to train for a wide range of healthcare scenarios while campuses are closed. Additionally, many campuses are offering their labs to assist the healthcare industry in their response to treating the Coronavirus. Respected associations and governing boards including the Society for Simulation in Healthcare and the International Nursing Association of Clinical Simulation have shared their support for “the use of virtual simulation as a replacement for clinical hours for students currently enrolled in health sciences professions (i.e. nursing students, medical students) during the current public health crisis caused by COVID-19. “
The hands-on training and exposure to treatment protocols will remain a necessity, and both virtual reality and simulation labs can augment the lack of clinical practice. Online simulations and previously recorded simulations are one option many programs are currently using during distance learning. With the return to campus, and as most simulation options will require in-person education, new student work protocols will be required. Considerations for PPE stations, new protocols for sanitation of materials (including VR headsets) and supplies as well as limitations on the number of students that can work in the lab at one time will all need to be taken into consideration. Last year, we shared a number of ideas and trends on this topic with College Planning & Management Magazine in our article “Experiential Learning in the Health Sciences.”
Over the next several weeks, we will stay close to this topic and address ways campuses may want to reconsider their program spaces going forward.
